As long ago as 1984, experimental programs were in place to deliver home-based phototherapy to healthy newborn babies with physiological jaundice.
Bilirubin levels were found to decrease just as rapidly in the home-based group as those treated in hospital, proving that home phototherapy can be a safe and effective alternative to hospital-based treatment (Eggert et al. 1985).
Despite these encouraging results, home-based care wasn’t routinely offered. Today, however, home-based phototherapy is once again emerging as a popular option for jaundiced infants who are otherwise healthy.

Inclusion Criteria
Note: Criteria may vary between organisations; refer to your local policies and procedures.
- Unconjugated hyperbilirubinaemia
- Total serum bilirubin (TSB) no greater than 50 micromol/L above the treatment line
- Conjugated bilirubin no greater than 10% of TSB.
The baby should:
- Be feeding well
- Be more than 24 hours of age
- Be greater than 37 weeks gestation
- Have a birth weight greater than 2500 grams.
Parents should be:
- Able to transport their baby to hospital if needed
- Confident to follow written and verbal instructions.
(QLD DoH 2022)
Exclusion Criteria
Not all cases of neonatal jaundice are suitable for home based-treatment. For example, the following criteria might preclude home treatment:
- Jaundice in the first 24 hours of life
- Poor feeding
- Temperature instability
- Lethargy
- Alloimmune haemolytic disease
- Asphyxia/acidosis
- Infection
- Abnormal liver function tests.
(QLD DoH 2022)
The following signs indicate a more serious case and might require emergency admission to a neonatal or paediatric unit:
- Jaundice with features of bilirubin encephalopathy (for example atypical sleepiness, poor feeding or irritability
- Jaundice first appearing at less than 24 hours of age.
(SCV 2023; RCHM 2020)
Other red flags include:
- Unwell neonate (for example, lethargy, fever, vomiting, irritability)
- Pale stools and dark urine (which could indicate (biliary obstruction)
- Weight loss of >10% within the first week of life
- Cephalohaematoma or bruising.
(RCHM 2020)
Phototherapy Blankets
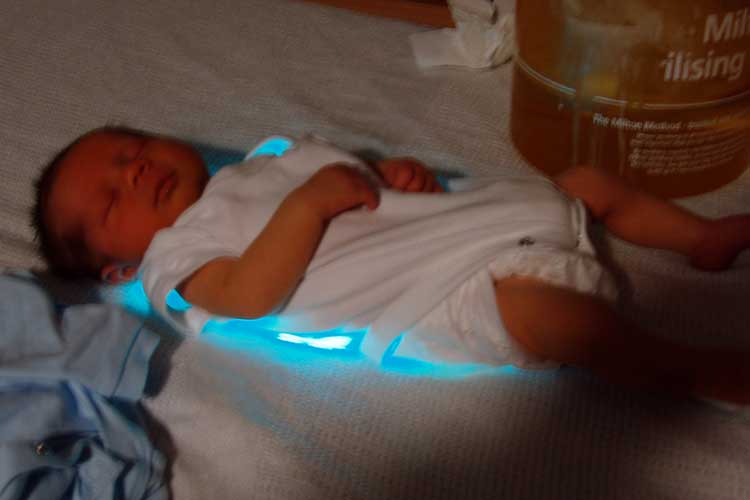
Today, home-based phototherapy delivered by light emitting diode (LED) phototherapy blankets is re-emerging as a popular option for home-based treatment. These blankets wrap around the baby for a prescribed length of time and allow them to be held, cuddled and fed as they normally would (NHS England 2018).
The use of these blankets helps prevent phototherapy from being interrupted during feeding and bonding (NHS England 2018).
Evaluating the Research
As with many medical innovations, although the evidence supporting home phototherapy is increasing, there is still a lack of good quality research to either support or refute treatment at home (Snook 2017).
One Cochrane review compared home-based phototherapy with hospital-based phototherapy for uncomplicated jaundice in full-term newborns, yet found no studies that met the eligibility criteria and concluded that there is currently insufficient high-quality evidence to either support or refute the use of home phototherapy for uncomplicated newborn jaundice (Malwade & Jardine 2014).
Home-Based Phototherapy Can Offer Significant Benefits
Increasing pressures on limited resources often result in innovation and the search for more cost-effective ways of delivering a service. Home-based phototherapy is a good example of this.
Hospital at home services allow resources to be used in a more effective way, cutting the costs of inpatient care and improving user satisfaction (NHS England 2018). For example, home-based phototherapy can result in:
- Better outcomes: A decrease in hospital admissions and reduction in the average length of stay for babies with neonatal jaundice.
- Better experience: Home-based care allows parents to have continued contact with their baby in their own home. Parents report feeling less stressed and more reassured about the quality of care provided.
- Better use of resources: Although home-based treatment requires an immediate financial outlay to purchase phototherapy blankets, there is also a corresponding reduction in the cost of using hospital resources.
(NHS England 2018)
This is an area where ongoing research is both timely and important, and studies such as the one conducted by Evelina London (2019) are paving the way forward. In this study, babies were considered for home treatment if they had been receiving phototherapy on the postnatal ward for at least 48 hours, had stable or falling bilirubin levels and could feed well.
The parents of these babies were trained to use the biliblanket and an outreach nurse from the neonatal unit visited them daily to test the babies’ bilirubin levels.
Conclusion

Whilst home phototherapy treatment is not yet considered routine, it could benefit many babies, providing the right training and safety measures are in place.
Topics
References
- Eggert, L, Pollary, R, Folland, D & Jung, A 1985. 'Home Phototherapy Treatment of Neonatal Jaundice', Pediatrics, vol. 76 no. 4, viewed 3 July 2023, https://pediatrics.aappublications.org/content/76/4/579
- Evelina London 2019, Helping Newborns With Jaundice To Go Home Earlier, Guy's and St Thomas' NHS Foundation Trust, viewed 3 July 2023, https://www.evelinalondon.nhs.uk/about-us/news-events/2019-news/20190402-helping-newborns-with-jaundice.aspx
- Jackson, C, Tudehope, D & Willis, L 2000, 'Home Phototherapy for Neonatal Jaundice - Technology and Team Work Meeting Consumer and Service Need', Australian Health Review, vol. 23 no. 2, viewed 3 July 2023, https://www.publish.csiro.au/ah/AH000162
- Malwade, U & Jardine, L 2014, 'Home- Versus Hospital-based Phototherapy for the Treatment of Non-haemolytic Jaundice in Infants at More Than 37 Weeks' Gestation', Cochrane Database of Systematic Reviews, viewed 3 July 2023, https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD010212.pub2/full
- NHS England 2018, 'Delivering Home Based Phototherapy to Babies With Physiological Jaundice', The Atlas of Shared Learning, viewed 3 July 2023, https://www.england.nhs.uk/atlas_case_study/delivering-home-based-phototherapy-to-babies-with-physiological-jaundice/
- Queensland Health 2022, Maternity and Neonatal Clinical Guideline: Neonatal Jaundice, Queensland Government, viewed 3 July 2023, https://www.health.qld.gov.au/__data/assets/pdf_file/0018/142038/g-jaundice.pdf
- The Royal Children's Hospital Melbourne 2020, Jaundice in Early Infancy, RCHM, viewed 4 July 2023, https://www.rch.org.au/clinicalguide/guideline_index/jaundice_in_early_infancy/
- Safer Care Victoria 2023, Jaundice in Neonates, Victoria State Government, viewed 4 July 2023, https://www.safercare.vic.gov.au/clinical-guidance/neonatal/jaundice-in-neonates
- Snook, J 2017, 'Is Home Phototherapy in the Term Neonate With Physiological Jaundice a Feasible Practice? A systematic Literature Review', Journal of Neonatal Nursing, vol. 23 no. 1, viewed 3 July 2023, https://www.sciencedirect.com/science/article/abs/pii/S1355184116300801?via%3Dihub
- Walls, M et al. 2004, 'Home Phototherapy In The United Kingdom', BMJ, viewed 3 July 2023, https://fn.bmj.com/content/89/3/F282.2
 New
New 
