In 2025, there have already been over 86,000 recorded influenza infections - over 10,000 more than the same time in 2024 (May 2025).
So, how can you best protect yourself this flu season?
What is Influenza?
Influenza (known colloquially as ‘the flu’) is a highly contagious, viral respiratory infection (NSW Health 2024).
Influenza infection in humans is most commonly caused by either type A or type B influenza viruses, and there are many sub-types and strains within each of these categories (NSW Health 2024).
Due to its high transmissibility, influenza often causes seasonal, widespread illness. In Australia, flu season typically lasts from April until September (Better Health Channel 2024).
On average, there are approximately 5,100 hospitalisations and 100 deaths caused by influenza every year in Australia (AIH 2025).
The symptoms of influenza can range from mild to serious illness with potentially life-threatening complications such as pneumonia, and can even result in death - even in people who are otherwise healthy (Better Health Channel 2024; AIH 2025).
Influenza is a vaccine-preventable illness (NSW Health 2024).
What Causes Influenza?

Influenza is spread through the respiratory fluids (from coughs and sneezes) of people who are infected with an influenza virus (Better Health Channel 2024).
It can be transmitted by:
- Breathing in respiratory droplets after an infected person has coughed or sneezed
- Making direct contact with fluid from an infected person’s coughs or sneezes
- Touching a surface that has been contaminated by respiratory fluids containing an influenza virus, then touching the eyes, nose or mouth.
(Healthdirect 2024; Queensland Government 2024)
People with influenza may be infectious from 24 hours prior to the onset of symptoms until one week after the onset of symptoms (although children and immunocompromised people might be infectious for longer) (Queensland Government 2024).
Symptoms of Influenza
Influenza often has a rapid onset of symptoms, which may include:
- Runny nose
- Sneezing
- Cough
- Sore throat
- Fever and chills
- Fatigue and weakness
- Reduced appetite
- Pain behind the eyes
- Headache
- Body aches
- Vomiting and diarrhoea (more common in children).
(Better Health Channel 2024; AIH 2025)
The typical timeline of symptoms is:
| Day 1-3 |
|
| Day 4 |
|
| Day 8 |
|
(Better Health Channel 2024)
Complications of Influenza
In some cases, influenza can lead to potentially severe complications, including:
- Pneumonia (primary viral and secondary bacterial pneumonia) - this is one of the most serious complications and can be life-threatening in older adults and people with chronic illness
- Acute bronchitis
- Croup
- Acute otitis media
- Asthma flare-up
- Acute respiratory distress syndrome
- Cardiac issues (e.g. myocarditis or pericarditis)
- Encephalitis and/or encephalopathy
- Reye syndrome
- Haematological abnormalities.
(AIH 2025; Mayo Clinic 2025)
Risk Factors for Influenza
Those identified as being at increased risk of contracting influenza and/or experiencing severe illness from influenza include:
- Older adults aged 65 and over
- Infants and children aged under 5 years
- Preterm infants aged under 37 weeks of gestation
- Aboriginal and Torres Strait Islander people
- Those who have never been exposed to an antigenically-related influenza virus
- Those infected with a highly virulent viral strain of influenza
- Those with certain chronic illnesses (e.g. Down syndrome, heart or lung disease, renal failure, diabetes, chronic neurological conditions)
- Those who are immunocompromised (e.g. due to HIV, being an organ transplant recipient or undergoing immuno-oncology therapy)
- Those with obesity (BMI ≥ 30 kg per m2)
- Those who are pregnant
- Those who smoke
- Those who are homeless
- Healthcare workers
- Those who are carers or household contacts of people in high-risk groups
- Residents, workers, volunteers and visitors at residential care facilities
- Workers in the commercial poultry and pork industry
- Those proving essential community services
- Travellers
- Children aged between 6 months and 10 years who are receiving long-term aspirin therapy.
(AIH 2025)
Diagnosis of Influenza
Influenza can be diagnosed through a polymerase chain reaction (PCR) test, in which a swab is taken from the nose and/or mouth (NSW Health 2024).
Treatment for Influenza
Mild cases of influenza will typically resolve on their own without treatment (Healthdirect 2022). Patients should be encouraged to rest, drink adequate fluids, take paracetamol to manage pain and fever, and use decongestant medicines to relieve their symptoms (Better Health Channel 2024).
Prescription antiviral medicines (such as oseltamivir) may be considered in patients who are moderately or severely ill or are at higher risk of serious illness from influenza (Immunisation Coalition 2024).
In more serious cases, patients may require admission to hospital (Better Health Channel 2024).
Influenza Vaccination
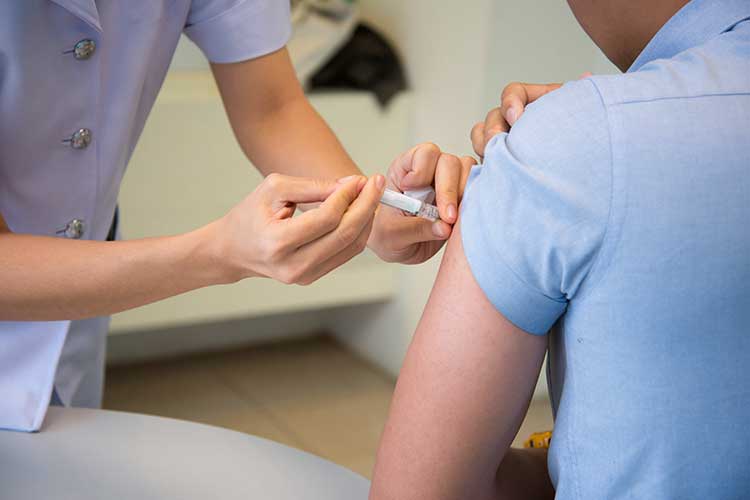
Vaccination is one of the best ways to prevent influenza (Better Health Channel 2024).
While the vaccine can’t guarantee prevention, it does provide a high level of protection against influenza and reduces the risk of severe illness if infection does occur (Better Health Channel 2024).
The Australian Immunisation Handbook (2025) states that all people aged 6 months and over should receive an influenza vaccine every year. This is because:
- The specific influenza virus strains included in the vaccine are different every year, depending on global influenza epidemiology
- Protection from the vaccine typically begins to decrease after three to four months.
Under the National Immunisation Program, certain vulnerable groups are eligible to receive the influenza vaccine for free.
Note: The influenza vaccine can be co-administered with a COVID-19 vaccine (AIH 2025).
When to Escalate Care
The following signs and symptoms in a person with influenza require immediate medical attention:
- Shortness of breath
- Chest pain
- Sudden dizziness
- Confusion
- Severe vomiting
- Fever accompanied by a rash
- Seizures
- Worsening of existing medical conditions
- Severe muscle pain or weakness
- Blue lips (in children)
- Dehydration (in children).
(Better Health Channel 2024; Mayo Clinic 2025)
Keep up-to-date with the latest influenza surveillance information on the National Notifiable Disease Surveillance System website.
Test Your Knowledge
Question 1 of 3
True or false: An influenza vaccine and a COVID-19 vaccine can be administered at the same time.
Topics
Further your knowledge
References
- Australian Immunisation Handbook 2025, Influenza (Flu), Australian Government, viewed 26 May 2025, https://immunisationhandbook.health.gov.au/vaccine-preventable-diseases/influenza-flu
- Better Health Channel 2024, Influenza (Flu), Victoria State Government, viewed 26 May 2025, https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/flu-influenza
- Healthdirect 2024, Flu (Influenza), Australian Government, viewed 26 May 2025, https://www.healthdirect.gov.au/flu
- Immunisation Coalition 2024, Antiviral Treatments for Influenza, Immunisation Coalition, viewed 26 May 2025, https://www.immunisationcoalition.org.au/resources/antiviral-treatments-for-influenza/
- May, N 2025, ‘Australia Has Had Record Flu Cases This Year – And That’s Before Winter Arrives. What’s Going On?’, The Guardian, 23 May, viewed 26 May 2025, https://www.theguardian.com/australia-news/2025/may/23/flu-record-cases-vaccination-australia
- Mayo Clinic 2025, Influenza (Flu), Mayo Clinic, viewed 26 May 2025, https://www.mayoclinic.org/diseases-conditions/flu/symptoms-causes/syc-20351719
- NSW Health 2024, Influenza Factsheet, New South Wales Government, viewed 26 May 2025, https://www.health.nsw.gov.au/Infectious/factsheets/Pages/influenza_factsheet.aspx
- Queensland Government 2024, Influenza (The Flu), Queensland Government, viewed 26 May 2025, http://conditions.health.qld.gov.au/HealthCondition/condition/14/217/82/Influenza-The-Flu
 New
New 

