More than 5 million Australians (one in four) experience bladder or bowel control problems (Healthdirect 2021; Continence Foundation of Australia 2022).
ot only can incontinence cause embarrassment, shame and even depression - in 2010, the cost of incontinence to Australia’s economy was approximately $42.9 billion, or $9,014 per patient (Deloitte Access Economics 2011).
Incontience can affect anyone, but 80% of those living with incontinence are women (Continence Foundation of Australia 2022).
Despite this, men are half as likely to seek care for incontinence as women (Clemens 2022), and one-third delay anti-incontinence surgery for over five years (Fuchs et al. 2018).
Incontinence Stigma and Shame
The loss of urine or faeces as an adult carries significant societal taboos. So strong is the taboo that people living with incontinence may have a negative body image and feel socially isolated (Continence Foundation of Australia 2020).
So, What is the Pelvic Floor, and How Can it Cause Incontinence?
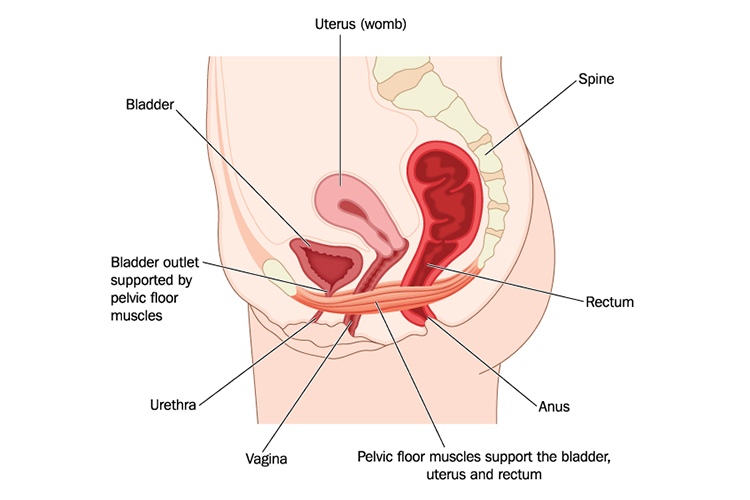
The pelvic floor is a sheet of muscles that extends from the coccyx (tail bone) to the pubic bone at the front of the body. This forms a platform between the legs and, as the name suggests, provides a floor to support the bladder and bowel.
The pelvic floor muscles also help to control the urethra and anus - allowing for the passage of urine and faeces out of the body. Female pelvic floor muscles also support the womb.
If the muscles are weakened, the supporting structures may lower into the vagina. Not only is this extremely uncomfortable, but it can also cause urinary or faecal incontinence.
Whilst pregnancy and childbirth are the common causes of pelvic floor weakening, it’s less well known that prostate surgery can also be a key cause.
Causes of a Weakened Pelvic Floor Include:
- Being overweight
- High impact exercise that overloads the pelvic floor muscles (e.g. weights-based or jumping activities)
- Certain surgeries (e.g. prostate surgery)
- Straining to open the bowels
- Chronic respiratory conditions or coughing
- Ageing
- Heavy lifting
- Pregnancy, childbirth and menopause.
(Better Health Channel 2021; POGP 2018)
Symptoms of a Weakened Pelvic Floor
When the pelvic floor muscles weaken, a range of symptoms can be experienced, such as:
- Stress urinary incontinence (leaking urine after a cough, sneeze or laugh)
- Increased frequency - needing to urinate repeatedly during the day and night
- Urge incontinence - a sudden and urgent need to visit the toilet, and often being unable to make it in time
- Nocturia - needing to get up to use the toilet during the night
- Inability to control the passing of wind
- A feeling of heaviness in the vagina
- Pain in the vaginal, abdominal or pelvic area
- Sexual dysfunction.
(Better Health Channel 2021; POGP 2018)
The Pelvic Floor and Sexual Function
Strengthening the pelvic floor muscles can improve sexual function.
Some pelvic floor muscles help to achieve erection and may prevent premature ejaculation (Wrightington, Wigan and Leigh Teaching Hospitals NHS Foundation Trust 2022).
For women, pelvic floor muscle strength is directly related to increased sensation and sexual function (POGP 2018).
Pelvic Floor Exercises

The thought of exercise and physical therapy can be difficult for patients to understand and incorporate into their lifestyle. Even though pelvic floor exercises can feel strange, no one can tell they’re being done - meaning they can be performed at any time or place.
By exercising the pelvic floor muscles, the structures can be supported again. Not only does this improve bowel and bladder control, but will also decrease or stop leakage.
Given the symptoms and consequences of incontinence, it’s perhaps quite staggering that simple and quick pelvic floor exercises can be so effective at preventing incontinence and reducing its impact.
One of the reasons why we might not exercise our pelvic floor muscles is the difficulty in locating exactly where they are. Being at the core of the body, they can be difficult to find, with confusion over whether you’re in the ‘right place’ or not.
One method of finding the pelvic floor muscles is to stop the flow of urine mid-stream. Note, however, that doing this frequently can be harmful, so it should not be used as an actual exercise technique (NHS 2020).
Once the pelvic floor muscles have been located, the exercise is straightforward: squeeze and draw in the muscles around the anus (and vagina for women), lift them up and hold for a count of eight, then let go. The length of the hold can be gradually built up from three to eight, or even higher, but it is vital that no other muscles are used.
It’s perhaps easier for women to exercise their pelvic floor, with the sheer amount of accessories and equipment that can be found from a quick online search. From ben wa balls to kegel devices, they are widely available and intensively marketed to women of a certain age. No wonder there is such a persistent stigma surrounding men suffering from pelvic floor weakness and incontinence issues.
Unfortunately, as these devices exercise the muscles from inside the vagina, it’s impossible for men to benefit, and there is no viable alternative for them.
With persistent exercise, the pelvic floor can be strengthened to reverse the weakening of the muscles, although full reversal may not be possible for all patients.
In such cases, there are other options available, including surgery.
It is important that everyone exercises their pelvic floor - even without symptoms and from a young age, as it is much easier to retrain previously strong muscles.
Conclusion
All efforts should be made to remove the stigma surrounding the ‘taboo’ topic of incontinence and encourage free and open discussion.
So, maybe when we’re checking for blood pressure and heart rate, we should also be having a conversation about pelvic floor exercises with our patients - regardless of their age or sex.
Test Your Knowledge
Question 1 of 3
True or false: Stopping the flow of urine mid-stream is an effective pelvic floor exercise that should be performed regularly.
Topics
References
- Better Health Channel 2021, Pelvic Floor, Victoria State Government, viewed 19 September 2023, https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/pelvic-floor
- Clemens, JQ 2022, Urinary Incontinence in Men, UpToDate, viewed 19 September 2023, https://www.uptodate.com/contents/urinary-incontinence-in-men
- Continence Foundation of Australia 2020, Psychological Impact, Continence Foundation of Australia, viewed 19 September 2023, https://www.continence.org.au/life-incontinence/caring-someone/psychological-impact
- Continence Foundation of Australia 2022, Understanding Incontinence, Continence Foundation of Australia, viewed 15 September 2023, https://www.continence.org.au/incontinence/understanding-incontinence
- Deloitte Access Economics 2011, The Economic Impact of Incontinence in Australia, Deloitte Access Economics, viewed 19 September 2023, https://agedcare.royalcommission.gov.au/system/files/2020-06/JOS.0001.0002.0001.pdf
- Fuchs, JS, Shakir, N, McKibben, MJ, Scott, JM & Morey, AF 2018, ‘Prolonged Duration of Incontinence for Men Before Initial Anti-incontinence Surgery: An Opportunity for Improvement’, Reconstructive Urology, vol. 119, viewed 19 September 2023, https://www.goldjournal.net/article/S0090-4295(18)30461-8/fulltext
- Healthdirect 2021, Incontinence: An Overview, Australian Government, viewed 15 September 2023, https://www.healthdirect.gov.au/incontinence
- National Health Service 2020, What are Pelvic Floor Exercises?, NHS, viewed 19 September 2023, https://www.nhs.uk/common-health-questions/womens-health/what-are-pelvic-floor-exercises/
- Pelvic, Obstetric and Gynaecological Physiotherapy 2018, The Pelvic Floor Muscles - a Guide for Women, POGP, viewed 19 September 2023, https://thepogp.co.uk/_userfiles/pages/files/resources/20818_pogp_pelvicfloor_for_women_signed_off_1.pdf
- Wrightington, Wigan and Leigh Teaching Hospitals NHS Foundation Trust 2022, Pelvic Floor Exercises For Male Patients, National Health Service, viewed 19 September 2023, https://www.wwl.nhs.uk/media/.leaflets/62d53abbecbfd8.04130905.pdf
 New
New 
