Caring for Clients With Corrective Lenses (Glasses and Contacts)
Published: 18 September 2023

Published: 18 September 2023

Vision disorders affect a significant number of Australians and the likelihood of developing a sensory problem only increases with age.
In Australia, about 55% of the population and 93% of people over the age of 65 are affected by a long-term vision disorder (AIHW 2023). Approximately 50% of Australians use corrective lenses (glasses or contacts) (AIHW 2016).
Given these statistics, it is almost certain that you will encounter clients who use corrective lenses, especially when caring for older adults.
Being able to ensure corrective lenses are being used appropriately is essential in keeping clients safe and enabling them to function in their daily lives.
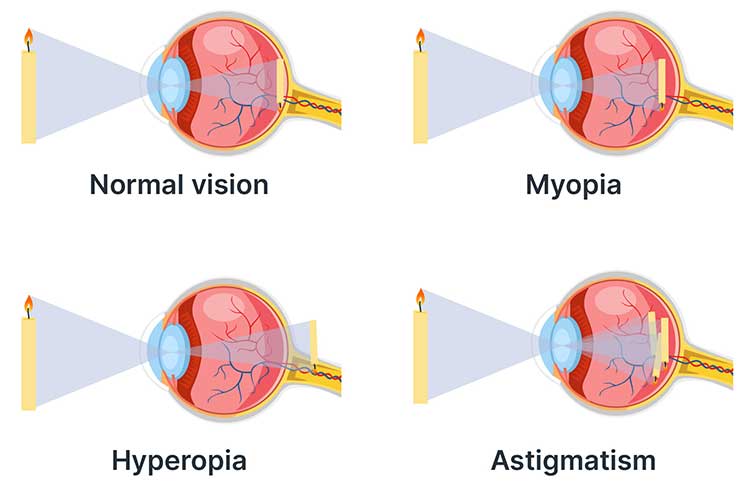
The majority of long-term vision disorders are refractive errors: hyperopia (long-sightedness), myopia (short-sightedness), astigmatism (blurred vision) and presbyopia (aged-related loss of focusing ability) (AIHW 2021).
Refractive errors occur when the shape of the eye is not able to bend light correctly, resulting in blurred vision. Corrective lenses such as glasses can be used to correct these errors. Generally, these conditions are hereditary or associated with ageing (Kellog Eye Center 2018).
The term vision impairment refers to vision loss caused by conditions, diseases or accidents. People with a vision impairment often have limited useful vision and may have difficulty performing day-to-day tasks. Unlike refractive errors, vision impairments are generally unable to be corrected by glasses (Visability 2023).
Refractive errors are generally considered disorders, but not disabilities. However, it is possible for them to lead to major vision loss or blindness (McManes 2023).
It’s important to ensure all clients are using their corrective lenses appropriately.
Clients who have an uncorrected refractive error may experience a variety of unwanted issues including:
(Fred Hollows Foundation 2020)
Those with very poor vision may experience more serious consequences, including:
(MDFA 2018)
For these reasons, it’s important to ensure clients are prescribed corrective lenses if they need them, and that clients who already have corrective lenses are actively using them with the right prescription.

Despite common vision disorders being easily correctable, there are several issues that can arise in care environments.
Clients in residential aged care often have poor awareness of their own vision and may not realise they are experiencing issues in the first place. As a result, they may not be prescribed the corrective lenses that they require (Cummins & Heraghty 2018).
Additionally, some clients with corrective lenses may have an outdated or incorrect prescription or stop wearing them altogether. Corrective lenses may be lost, broken, scratched or dirtied and clients will not necessarily speak up if this happens (Cummins & Heraghty 2018; Kell 2017).
The accidental switching of glasses between clients is also possible, especially in residential aged care settings where clients may mistakenly pick up and keep someone else’s glasses (Cummins & Heraghty 2018).
In some cases, a client may have an incorrect prescription due to changes in vision over time, human error or inaccurate readings during an eye examination. Someone who has an incorrect prescription may experience blurred vision, dizziness, headaches, eye strain or other symptoms similar to those experienced when not wearing corrective lenses (Win 2023).
Glasses should fit correctly. When checking a client’s glasses, ensure that:
(Belden 2019)
Read: Sensory Loss in Older Adults

The following tips will help ensure your clients are using corrective lenses properly and are referred to an optometrist if required.
(MDFA 2018; Healthdirect 2021)
Corrective lenses are an easy way to treat common vision disorders. However, it is important to check that clients’ glasses and contact lenses fit appropriately, are the correct prescription and are being used by the right person. If there are any concerns or sudden changes in vision, the client should be referred to an eye specialist.
This will ensure clients are able to go about their daily activities comfortably and safely.
Question 1 of 3
How many Australians use corrective lenses?