Fungal Nail Infections
Published: 16 October 2023
Published: 16 October 2023

Fungal nail infection, also known as onychomycosis, is a cause of embarrassment and discomfort for millions of people worldwide. These infections are often very difficult to treat and full resolution may take more than a year (CDC 2022).
While anyone can contract a fungal infection of the nails, older adults are more commonly affected (CDC 2022). In western countries, approximately 10% of adults under the age of 60 have a fungal nail infection. After the age of 60, this increases to 20% (Han & Stöppler 2023).
Factors that promote the occurrence of fungal infections include working in warm damp environments, wearing closed shoes, using public pools and gyms, and having family members with nail infections. Men tend to have higher rates of infection than women (Han & Stöppler 2023; Kahn & Luo 2023).
Illness and medical treatments also increase the risk. Individuals who are diagnosed with psoriasis or psoriatic arthritis are more prone to fungal infections. People with skin diseases, including eczema and athlete’s foot, have an elevated risk. Conditions such as diabetes and peripheral vascular disease that impair the body’s ability to fight infection also increase the risk. Individuals who have sustained injuries to their fingers or toes are more prone (Han & Stöppler 2023).
Medications that weaken the immune system such as chemotherapy make it easier for fungi to infect nails. Steroids, surgery, and radiation all lower resistance to disease and increase the risk of nail infections (CDC 2020, 2022; Han & Stöppler 2023).
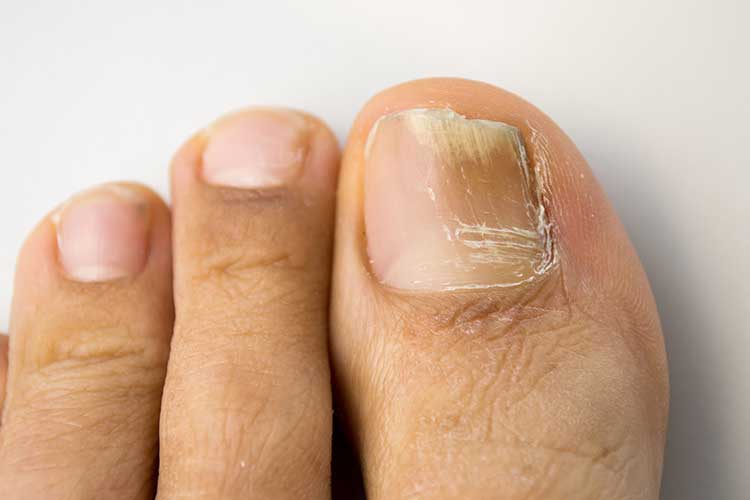
The signs of a fungal nail infection vary, but can include:
(Mayo Clinic 2022; Han & Stöppler 2023; NHS 2021)
If the fungal infection remains untreated, it may spread to other areas of the body, or secondary bacterial infection may ensue and the nail may become permanently deformed or destroyed (Kahn & Luo 2023).
Fungal nail infections are difficult to treat. The entire nail must grow out before treatment can be clearly identified as a success, which may take up to 12 months (Han & Stöppler 2023).
Patients may ask you about home remedies. Most of these are ineffective; some are merely cumbersome while others can cause damage to the nails and surrounding tissues. People sometimes use bleach, vinegar, mouthwash, or hydrogen peroxide to treat their infections. Healthcare professionals must be prepared to discourage the use of these treatments.
Over-the-counter medicines are not considered reliable as they may be unable to effectively penetrate the nail (Han & Stöppler 2023).
Other problems faced by users of topical remedies are inconsistent use and recontamination.
Topical prescription remedies are also considered a less effective treatment method. However, compared to oral treatments, there is a decreased risk of side effects and medicine interactions (Han & Stöppler 2023).
Oral antifungal agents are the most effective treatment method for fungal nail infections. However, even though they have a higher cure rate, it is still possible for the infection to return, even after successful treatment (Han & Stöppler 2023).
Oral treatments are also associated with potentially severe side effects including headaches, itching, diarrhoea, and loss of taste. They are unsuitable for pregnant patients and may cause liver damage in some cases (NHS 2021).
Debridement of a partial or entire nail may be accomplished by chemical or surgical means. This is performed in conjunction with the use of topical and, sometimes, oral agents.
Laser therapy may be used to destroy the fungus; however, it appears to be less effective than other methods (NHS 2021; Healthdirect 2022).
Effective treatment of this uncomfortable and embarrassing ailment relies on increased awareness and education being provided to patients so that fungal nail infections are treated promptly. Further research is needed to develop safer, faster, economical and more effective treatments for this common condition.